
Jul 28, 2023 | Uncategorized
LATISSE® is a prescription medication used to treat hypotrichosis, a condition that results in inadequate eyelash growth. It contains an active ingredient called bimatoprost, which helps to promote the growth of longer, thicker and darker eyelashes.
To use LATISSE®, a thin line of the solution is applied to the base of the upper eyelashes once a day. It is important to follow the application instructions carefully, as using too much or too often can lead to side effects such as redness, itching, and darkening of the skin around the eyes.
Although rare, more serious side effects can occur with LATISSE®, such as changes in eye color or eyelid skin darkening. It is important to talk to your doctor if you experience any unusual symptoms or if you have a history of eye problems.
Despite the potential for side effects, LATISSE® has been shown to be an effective treatment for hypotrichosis, helping many people to achieve longer, thicker and more beautiful eyelashes. If you are interested in using LATISSE®, schedule an appointment with Dr. Neily to determine if it is the right treatment option for you.

Jul 21, 2023 | Uncategorized
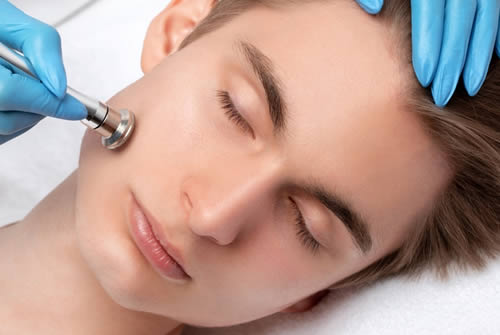
Facial chemical peels have become an increasingly popular cosmetic procedure in recent years. This non-invasive treatment involves the application of a chemical solution to the face, which exfoliates and removes the outermost layers of skin. The result is smoother, brighter skin with a more even tone and texture.
Chemical peels can be used to treat a variety of skin conditions, including acne, hyperpigmentation, fine lines and wrinkles, and uneven skin tone. They work by stimulating cell turnover and collagen production, which helps to rejuvenate the skin. There are three main types of chemical peels: superficial, medium-depth, and deep. The type of peel used will depend on the individual’s skin concerns and desired outcome.
While chemical peels are generally safe and effective, there are potential side effects to be aware of. These may include redness, peeling, and sensitivity to the sun. It is important to follow proper aftercare instructions to minimize the risk of complications.
Overall, facial chemical peels are a popular and effective option for those looking to improve the appearance of their skin. Call us at Coast Dermatology to determine if this treatment is right for you.
Aug 28, 2023 | Uncategorized
Dermabrasion is a cosmetic dermatology procedure that involves removing the top layer of skin to improve the appearance of fine lines, wrinkles, acne scars, and other skin imperfections. During the procedure, a special device is used to gently exfoliate the skin, revealing a smoother, more even complexion. The device is a special wand with a rotating, abrasive surface that is used to remove the top layer of skin. This wand is typically made of a wire brush or diamond wheel and is attached to a motorized handle. The wand is moved across the skin in a controlled manner, allowing the abrasive surface to slough off dead skin cells and other debris. The depth of the treatment is determined by the pressure applied to the wand and the length of time it is used. The wand can be adjusted to treat delicate areas of the face or more resilient areas of the body, making it a versatile tool for cosmetic dermatologists.
Dermabrasion can be used to treat a range of skin concerns, including age spots, hyperpigmentation, and rough or uneven skin texture. It is typically performed on the face but can also be used on other parts of the body.
While dermabrasion is generally safe, there are some potential side effects to be aware of. These may include redness, swelling, and sensitivity to the sun. It is important to follow your dermatologist’s aftercare instructions, including using sunscreen and avoiding sun exposure, to minimize the risk of complications.
Overall, dermabrasion is a popular and effective treatment option for those looking to improve the appearance of their skin. If you are interested in dermabrasion, contact us at Coast Dermatology to schedule an appointment.

Aug 7, 2023 | Blog
BOTOX® is a well-known cosmetic treatment that has become increasingly popular in recent years. It is an injectable medication that is used to relax the muscles in the face, reducing the appearance of fine lines and wrinkles. The active ingredient in BOTOX® is botulinum toxin, which is a neurotoxin that temporarily paralyzes the muscles that cause wrinkles. BOTOX® is commonly used in cosmetic dermatology to treat wrinkles on the forehead, between the eyebrows, and around the eyes, such as crow’s feet. The treatment takes only a few minutes and involves a series of small injections. Results typically last for three to four months, after which the treatment can be repeated. One of the main advantages of BOTOX® is that it is a non-surgical option for reducing the signs of aging, making it a popular choice for those who want to improve their appearance without undergoing surgery. While BOTOX® is generally considered safe, there are some potential side effects to be aware of. These may include temporary bruising, redness, or swelling at the injection site. In rare cases, patients may experience headaches, nausea, or flu-like symptoms. In even rarer cases, patients may experience drooping eyelids or eyebrows, although this usually resolves on its own within a few weeks. It’s important to choose a qualified and experienced provider for your BOTOX® treatments, as this can help minimize the risk of side effects. Dr. Neily can also help you understand what to expect before, during, and after your treatment, and can answer any questions you may have about the procedure. Call us to schedule your BOTOX® appointment today.
May 14, 2023 | Blog
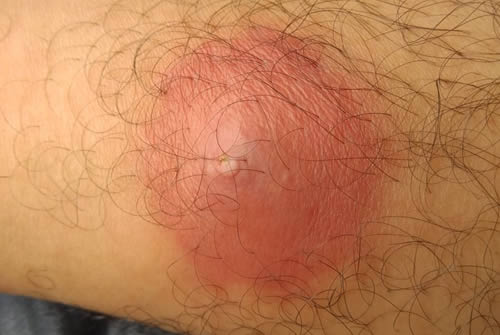
Abscesses, commonly referred to as boils, are inflamed lumps that emerge beneath the skin and can be quite painful. These boils result from infections in hair follicles or oil glands. Boils can appear on any part of the body, but they are often found on the neck, face, buttocks, thighs, and armpits.
Causes of Boils
Boils are mainly caused by Staphylococcus aureus, a bacterium that usually resides on the skin and inside the nose, but can infiltrate the body through a wound or skin breakage. Other bacterial strains such as Streptococcus pyogenes can also cause boils. The risk factors for boils development include:
- Poor hygiene
- Diabetes
- Exposure to harsh chemicals
- Weakened immune system
- Friction from shaving or wearing tight clothes
- Certain medications like steroids
Symptoms of Boils
Boils commonly start as red, tender bumps that progressively grow in size within a few days. The sizes of boils can range from a pea size to a golf ball. They may be accompanied by a fever or feeling of general illness. As the boil expands, it may develop a yellow or white center, which is pus that has collected beneath the skin. The skin over the boil may also be tender and swollen.
Types of Boils
Various types of boils include:
- Furuncles: single boils that manifest on the skin and are often caused by Staphylococcus aureus.
- Carbuncles: clusters of boils that are typically more massive than furuncles and can cause significant pain. Carbuncles are also more likely to induce a fever or other systemic symptoms than furuncles.
- Cystic acne: deep, inflamed, and painful cysts that occur on the neck, face, chest, and back due to clogged hair follicles.
Treatments for Boils
Most boils tend to heal without treatment within several weeks. Nonetheless, some treatments can help to alleviate the pain and quicken the healing process. They include:
- Applying warm compresses to the affected area for several minutes multiple times a day.
- Taking over-the-counter painkillers such as acetaminophen or ibuprofen to reduce inflammation and alleviate pain.
- Keeping the affected region clean and dry to prevent further infection.
- Taking antibiotics if the boil is severe or there are multiple boils.
- In rare cases, a boil may need to be drained by a healthcare professional. This involves making a small incision in the skin and draining the pus out of the boil.
Preventing Boils
Several measures can be taken to prevent the development of boils, such as:
- Practicing good hygiene, such as washing hands frequently and showering after heavy sweating or exercise.
- Avoiding sharing personal items like towels, razors, or clothing.
- Avoiding tight-fitting clothes that can cause skin friction.
- Promptly treating any cuts or breaks in the skin with antiseptic to prevent infection.
Boils can be uncomfortable and painful, but they are usually not a serious cause for concern. Good hygiene practices and measures to prevent the development of boils can help to keep your skin healthy and infection-free. Most boils tend to heal on their own within a few weeks, but if the boil does not heal or you experience symptoms of a severe infection, it is important to seek medical attention. Contact Dr. Neily at our Venice dermatology office to schedule an appointment.
May 21, 2023 | Blog
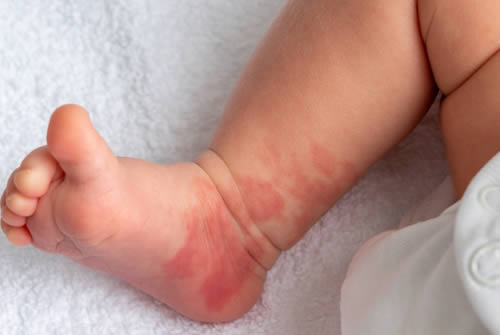
Birthmarks are a common occurrence in newborns and are characterized by an overgrowth of skin pigment cells or blood vessels. While most birthmarks are benign, some may indicate an underlying medical condition. The exact cause of birthmarks is still unknown, although some factors may increase the likelihood of developing them, such as genetics and certain medical conditions.
There are two primary types of birthmarks: pigmented and vascular.
Pigmented Birthmarks:
Café-au-lait Spots: These spots are typically present at birth and are flat, light brown in color.
Mongolian Spots: These blue-gray patches of skin are typically found on the lower back or buttocks.
Moles: Moles are clusters of pigment cells and can vary in color, size, and shape.
Vascular Birthmarks:
Port-wine Stains: These red or purple birthmarks are caused by abnormal blood vessel growth.
Strawberry Hemangiomas: These raised, red birthmarks usually appear within the first few weeks of life.
Salmon Patches: These pink birthmarks are typically flat and can be found on the forehead, eyelids, or neck.
Treatment options for birthmarks depend on the type and severity of the birthmark. While most birthmarks do not require treatment and will fade over time, some may cause discomfort or be a sign of an underlying medical condition. Here are some common treatments for birthmarks:
Laser Therapy: This treatment uses lasers to target and destroy the blood vessels or pigment cells in the birthmark.
Surgery: In some cases, surgical removal may be necessary.
Medications: Certain medications can help to shrink or reduce the appearance of birthmarks.
It is important to consult with a dermatologist if you have concerns about a birthmark. Although most birthmarks are harmless, some may require treatment if they are causing discomfort or indicate an underlying medical condition. Dr. Neily, a board-certified dermatologist in Venice, Florida can provide expert guidance and care. Contact us today to schedule an appointment.

May 27, 2023 | Blog
Pregnancy is a time of joy and excitement for women, but it also brings about changes in the skin. Due to hormonal fluctuations, various skin conditions can arise during pregnancy that can be uncomfortable, painful, and irritating. Luckily, there are treatments available to alleviate these conditions, and a dermatologist can help with the process. Let’s take a look at some of the most common skin conditions during pregnancy and the recommended dermatology treatments for each.
Melasma:
Melasma is a skin condition that frequently occurs during pregnancy due to hormonal changes. Dark patches appear on the face, especially on the cheeks, nose, forehead, and upper lip. To treat melasma, dermatologists usually suggest topical creams containing hydroquinone, corticosteroids, or tretinoin. Other options include microdermabrasion, chemical peels, and laser therapy, which can reduce the visibility of dark spots.
Acne:
Hormonal changes during pregnancy can worsen acne. Dermatologists may suggest benzoyl peroxide or salicylic acid for topical treatment. Depending on the acne’s severity, other medications such as oral antibiotics or other prescription medicines may be prescribed.
Pruritic Urticarial Papules and Plaques of Pregnancy (PUPPP):
PUPPP is a common skin condition that appears during the third trimester of pregnancy. It creates red, itchy, and raised bumps on the skin, particularly on the thighs, abdomen, and buttocks. Antihistamines and topical steroids can help relieve PUPPP-related itching.
Papular Eruptions of Pregnancy:
Papular Eruptions of Pregnancy (PEP) is another common skin condition that occurs during pregnancy. It causes itchy red bumps to appear on the skin, usually on the arms, legs, and abdomen. Topical steroids, oral antihistamines, or UV light therapy are typical treatments for PEP.
Pemphigoid Gestationis:
Pemphigoid Gestationis (PG) is an autoimmune disorder that is rare but can develop during pregnancy. The skin develops itchy, blistering lesions that typically begin around the belly button and can spread to other areas of the body. Treatment involves the use of topical and/or oral steroids to reduce inflammation and suppress the immune system.
Intrahepatic Cholestasis:
Intrahepatic Cholestasis of Pregnancy (ICP) is a liver disorder that occurs during pregnancy. It causes intense itching on the hands and feet and can be associated with jaundice. Doctors generally prescribe medications to relieve itching and monitor liver function. Delivery may also be suggested, as the condition can worsen in the later stages of pregnancy.
If you’re suffering from any of these skin conditions during pregnancy, it’s essential to consult with a dermatologist. Dr. Neily in Venice, Florida is available to diagnose the condition and recommend the best treatment options to ensure the health of both you and your baby. Contact us today!
Jun 7, 2023 | Blog
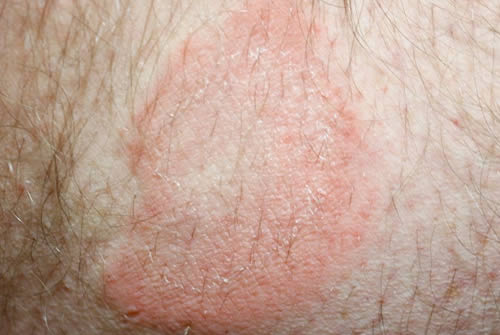
Granulomas refer to small areas of inflammation that develop in response to irritants, infections, or foreign substances in various tissues of the body. These clusters of immune cells, such as macrophages, gather together to contain the irritant. In this article, we’ll take a closer look at the symptoms, causes, types, and treatments of granulomas.
Causes of Granulomas
Several factors can lead to the formation of granulomas, including infections, inflammation, autoimmune diseases, and exposure to foreign substances. Some of the most common causes of granulomas include:
- Infections such as tuberculosis, fungal infections, and leprosy
- Autoimmune diseases such as Crohn’s disease and sarcoidosis
- Exposure to foreign substances such as talcum powder or silicone
- Chronic inflammation due to conditions such as rheumatoid arthritis or inflammatory bowel disease
Symptoms of Granulomas
The symptoms of granulomas may vary depending on the location and cause of the granuloma. In some cases, they may not cause any symptoms at all. However, common symptoms of granulomas include:
- Bumps or lesions on the skin
- Fatigue
- Coughing
- Shortness of breath
- Joint pain or stiffness
- Weight loss
- Abdominal pain or discomfort
Types of Granulomas
There are several types of granulomas, which include:
- Tuberculoid granulomas: Caused by tuberculosis or other mycobacterial infections and characterized by a central area of caseation necrosis surrounded by immune cells.
- Foreign body granulomas: Develop in response to foreign substances that cannot be broken down by the body, such as talcum powder or silicone.
- Sarcoid granulomas: Characteristic of sarcoidosis, an autoimmune disease where immune cells cluster together in organs like the lungs, lymph nodes, and other areas.
- Granulomatous vasculitis: An inflammatory condition that affects blood vessels, leading to the formation of granulomas around vessel walls.
Treatments for Granulomas
The treatment of granulomas depends on the underlying cause and severity of symptoms. Treatment options include:
- Antibiotics or antifungal medication for infections
- Steroids or immunosuppressive medication for autoimmune diseases
- Surgical removal of foreign bodies
- Injections of corticosteroids into the affected area to reduce inflammation and promote healing
In some cases, granulomas may not require treatment and may go away on their own. If you have symptoms of a granuloma, it is important to seek medical attention to determine the underlying cause and appropriate treatment plan. Call our Venice office and schedule an appointment with Dr. Neily today!
Jun 14, 2023 | Blog
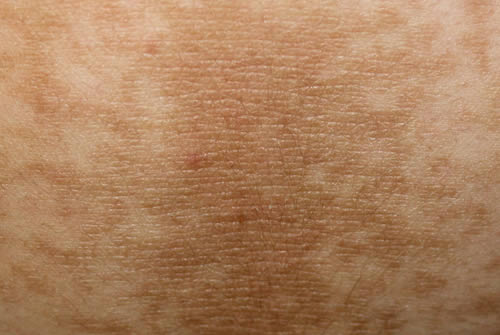
Acanthosis nigricans is a skin condition characterized by the presence of dark, velvety patches on the skin, typically found on the neck, armpits, groin, and other skin folds. The patches may also appear on the hands, elbows, knees, or face. The affected skin is often thick, rough, and itchy. This condition affects both men and women of any age, although it is more prevalent in those who are overweight, have insulin resistance or type 2 diabetes.
The main cause of acanthosis nigricans is an increase in insulin levels. High insulin levels can stimulate skin cell growth and trigger melanin production. Obesity, insulin resistance, type 2 diabetes, hormonal disorders such as polycystic ovary syndrome, or certain medications can contribute to the increase in insulin levels that cause acanthosis nigricans.
The symptoms of acanthosis nigricans include the presence of dark, thick, velvety patches of skin on the neck, armpits, groin, and other skin folds. The skin may feel rough and itchy, and in some cases, may emit a foul odor.
There are different types of acanthosis nigricans, including type 1, which occurs in people with insulin resistance, usually due to obesity or type 2 diabetes, type 2, which occurs in people who do not have insulin resistance or diabetes but have a genetic predisposition to the condition, and drug-induced, which occurs as a side effect of certain medications.
While there is no specific cure for acanthosis nigricans, treatment options are available. Treating the underlying cause, such as losing weight and improving blood sugar control for people with insulin resistance or type 2 diabetes, can help improve the condition. Medications or topical treatments may be prescribed to help reduce the appearance of the patches. Dermabrasion, laser therapy, and chemical peels are also used to improve the appearance of affected skin.
Preventing the development of acanthosis nigricans includes maintaining a healthy weight, exercising regularly, and eating a healthy diet. Managing any underlying medical conditions, such as diabetes or hormonal disorders, can also help prevent the condition. If you notice any changes in your skin, especially in the skin folds, consult with Dr. Neily at Coast Dermatology for an early diagnosis and treatment to prevent the condition from getting worse.
Jun 21, 2023 | Blog
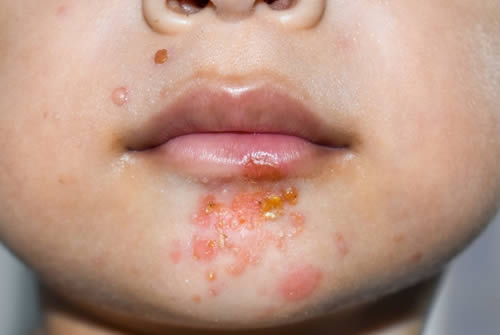
Impetigo is a bacterial skin infection that is contagious and commonly affects children, but it can occur at any age. This infection can spread easily among children in close contact, such as in schools and daycare centers. If you suspect that you or your child has impetigo, it is essential to seek medical attention from a dermatologist who can diagnose and treat the condition.
The symptoms of impetigo are red sores or blisters that appear on the face, neck, hands, and other areas of the body. The sores may burst and develop yellow-colored crusts that can be itchy and uncomfortable. Impetigo can also cause swollen lymph nodes, particularly in the affected area. In severe cases, impetigo can cause fever and chills.
Antibiotics are the most common treatment for impetigo, either applied topically or taken orally. The type of antibiotic prescribed will depend on the severity of the infection and other factors. Completing the full course of antibiotics is crucial, even if the symptoms improve or disappear, to prevent the infection from recurring.
Aside from the treatments mentioned above, it is important to take measures to prevent the spread of impetigo. Here are some tips to remember:
- Keep the affected areas clean: Clean the affected areas with soap and water regularly. This can help remove the crusts and prevent the bacteria from spreading.
- Avoid touching the affected areas: Try to avoid touching the affected areas as much as possible. If you do touch them, make sure to wash your hands thoroughly with soap and water.
- Cover the affected areas: Cover the affected areas with a clean, dry bandage or gauze to prevent the spread of the bacteria to other parts of your body or to other people.
- Don’t share personal items: Avoid sharing personal items such as towels, clothing, or bedding with others, as this can spread the bacteria.
- Practice good hygiene: Good hygiene habits, such as washing your hands regularly, can help prevent the spread of impetigo and other infections.
If you suspect that you or someone in your family has impetigo, it is important to seek medical attention as soon as possible. A dermatologist can help diagnose and treat impetigo, as well as provide guidance on how to prevent its spread. With prompt and effective treatment, most cases of impetigo can be resolved within a few weeks. Make an appointment with Dr. Neily Board Certified dermatologist today.
Jun 27, 2023 | Blog
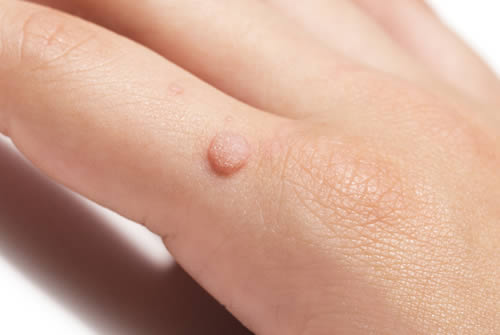
Warts are benign growths on the skin caused by the human papillomavirus (HPV). They can occur on any part of the body, but most commonly appear on the hands, feet, and face. Warts can be spread through direct contact with an infected person or surface.
Common causes of warts include a weakened immune system and skin damage such as cuts, abrasions, or cracks. There are several types of warts including common warts, plantar warts, flat warts, filiform warts, and genital warts. Symptoms of warts can include small, rough growths on the skin, discoloration, tenderness, itching, and irritation.
Various treatments are available for warts, including over-the-counter medications containing salicylic acid, prescription medications like imiquimod cream, cantharidin, podophyllin, or retinoid cream, as well as surgical removal, laser treatment, freezing or burning by a doctor or dermatologist. To prevent warts, avoid direct contact with infected skin or surfaces, keep the skin clean and dry, avoid picking at warts, wear protective footwear in public places, and strengthen your immune system by eating a healthy diet and exercising regularly.
If you suspect that you have a wart or are experiencing any of the associated symptoms, consult with a board-certified dermatologist such as Dr. Neily, who can provide a proper diagnosis and recommend the best treatment options for your individual needs. Call our office today to schedule an appointment.

Jul 7, 2023 | Blog
Skin cancer is a pervasive problem in the US, with millions of people being affected by it each year. Detecting and treating it early is crucial to its management, which is why regular skin cancer checks with a dermatologist are vital.
A skin cancer check is a non-invasive examination that can identify early signs of skin cancer. During the checkup, a dermatologist will assess the entire body, including the scalp, nails, and the spaces between the toes and fingers. They will look for any abnormal spots, moles, or freckles on your skin.
To identify any suspicious areas, the dermatologist will evaluate the size, shape, color, and texture of each spot on your skin. They may also use a dermatoscope, a device that illuminates and magnifies the skin to examine any unusual spots in greater detail. They will ask about any symptoms, such as itching, pain, or bleeding, that you may be experiencing. The doctor will also ask about your medical history and any family history of skin cancer to determine your risk level for skin cancer.
If the dermatologist detects any suspicious areas, they may suggest a skin biopsy. There are various types of skin biopsies available, such as shave biopsies, punch biopsies, and excisional biopsies, depending on the size and location of the questionable region. It is critical to keep in mind that early detection is crucial for skin cancer, so do not hesitate to contact us at Coast Dermatology and Skin cancer Center if you have any concerns or notice any changes in your skin. Book an appointment with Dr. Neily, a Mohs Micrographic Surgeon, for a skin cancer check today.

Jul 14, 2023 | Blog
Summertime is a wonderful season to bask in the sun and relax, but the sun’s intensity also heightens. While most people appreciate a sun-kissed glow, exposure to the sun’s harmful ultraviolet (UV) rays can cause severe skin damage like sunburn, premature aging, and skin cancer. As a matter of fact, skin cancer is the most frequent form of cancer diagnosed in the United States, with over 9,000 cases every day. The good news is that it is easy to take a few steps to protect yourself from the sun and maintain a healthy and radiant complexion throughout the year.
Tip #1: Wear Protective Clothing
One of the most efficient methods to safeguard your skin from the sun is to cover up. Put on long-sleeved shirts, pants, and wide-brimmed hats to shield your skin from direct sunlight. Furthermore, look for clothing with built-in UPF (Ultraviolet Protection Factor) to provide more extensive protection from harmful rays.
Tip #2: Apply Sunscreen
Sunscreen is a necessary element of sun protection. It is recommended to use a broad-spectrum sunscreen with an SPF (Sun Protection Factor) of at least 30. Apply sunscreen generously to all exposed skin and reapply every two hours or more frequently if you are swimming or sweating. Remember to apply sunscreen to commonly neglected areas such as your ears, hands, and feet.
Tip #3: Find Shade
Seeking shade is a simple yet effective way to shield yourself from the sun. Refrain from spending time outdoors during the hours when the sun is at its peak, typically between 10 a.m. and 4 p.m. When outside, search for a shaded area, such as under a tree or umbrella, to reduce your exposure to UV rays.
Tip #4: Be Aware of Reflective Surfaces
Reflective surfaces such as water, sand, and snow can increase your exposure to UV rays. When spending time near these surfaces, be sure to take extra precautions by wearing protective clothing, applying sunscreen, and finding shade.
Tip #5: Protect Your Eyes
UV rays can cause damage to your eyes as well as your skin. Guard your eyes by wearing sunglasses with UV protection. This will not only protect your eyes from harmful rays but also help reduce the risk of cataracts and other eye conditions.
Shielding yourself from the sun is crucial for maintaining healthy skin and reducing the risk of skin cancer. By following these simple tips, you can enjoy all the benefits of the sun without putting your health at risk. Remember, prevention is crucial, so make sure to protect your skin from the sun every day. Schedule your next skin cancer check with Dr. Neily at Coast Dermatology and Skin Cancer Center today!
Aug 21, 2023 | Blog
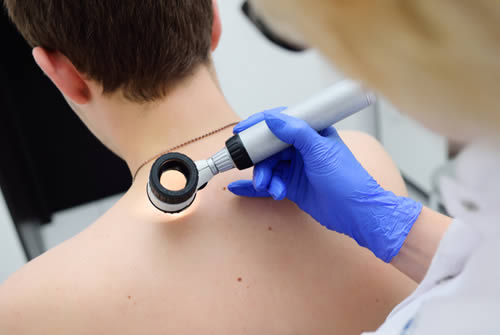
Moles are a type of skin growth that is common in many people. They are formed by clusters of pigment-producing cells called melanocytes. Although most moles are harmless, it is important to know the different types and be aware of any changes to them. Moles generally appear as a single shade of color, ranging from beige to dark brown, and have a well-defined border. However, moles can develop during any stage of life and may darken with sun exposure or hormonal changes.
There are several types of moles, including:
- Junctional nevus: These moles are typically round or oval with a flat surface and can appear at any age.
- Compound nevus: These moles have a raised surface and are brown in color.
- Dermal nevus: These moles are usually skin-colored and have a raised surface.
- Blue nevus: These moles are typically blue or blue-gray and can appear anywhere on the body.
- Halo nevus: These moles are surrounded by a white ring or halo and can appear at any age.
It is important to monitor any changes to moles, as this can indicate skin cancer. Signs of concern include:
- A mole that changes color, shape or size
- A mole that is larger than a pencil eraser
- A mole that is asymmetrical or has an irregular border
- A mole that is itchy or painful
- A mole that bleeds or oozes
If a mole is causing discomfort or there is a risk of skin cancer, it may need to be removed by a dermatologist. Depending on the type of mole, the dermatologist may use surgical excision, laser surgery or shave removal.
Protecting your skin from sun damage is an important step in preventing skin cancer. Here are some tips to reduce exposure to the sun:
- Wear protective clothing, such as long-sleeved shirts and hats
- Apply sunscreen with a minimum SPF of 30 to all exposed skin
- Limit time in the sun, especially during peak hours
- Avoid tanning beds
Overall, it is important to be aware of any changes to moles and take steps to protect your skin from the sun. If you have concerns about a mole or notice any changes, consult with Dr. Neily Venice Board Certified dermatologist for proper diagnosis and treatment.
Aug 14, 2023 | Blog
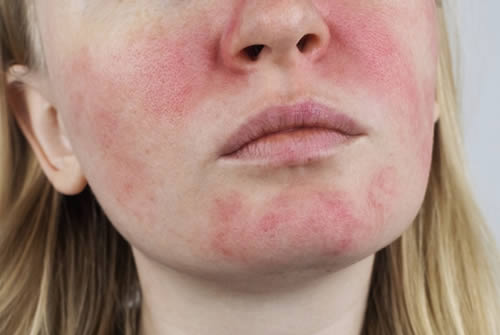
Rosacea is a chronic skin condition that affects a significant number of people globally. It is characterized by the presence of redness, flushing, and visible blood vessels on the face, mainly on the forehead, cheeks, nose, and chin. Rhinophyma, thickened skin on the nose, papules, and pustules are other common symptoms of this condition. Rosacea tends to affect fair-skinned individuals and women over the age of 30, but it can occur at any age and affect anyone.
At Coast Dermatology in Venice, FL, Dr. Neily, a Board Certified Dermatologist, provides comprehensive care for rosacea. He works closely with his patients to identify the triggers that exacerbate their symptoms and create a customized treatment plan. While there is no cure for rosacea, it is possible to control the symptoms and prevent flare-ups.
The first step in managing rosacea is to avoid triggers that worsen the condition. Sun exposure, spicy foods, alcohol, heat, and stress are some of the most common triggers. Patients should use mild skincare products that do not irritate the skin and avoid harsh exfoliants and abrasive scrubs. A good skincare routine for rosacea should include a mild cleanser, fragrance-free moisturizer, and a broad-spectrum sunscreen.
If changes to lifestyle and skincare products do not provide the desired relief, prescription medications may be necessary. Topical antibiotics like metronidazole, azelaic acid, and ivermectin reduce inflammation and kill bacteria on the skin. Topical retinoids like tretinoin and adapalene improve skin texture and reduce redness by regulating cell turnover. Oral antibiotics like tetracycline, doxycycline, and minocycline are prescribed for severe cases to kill bacteria from the inside out and reduce inflammation. Laser therapy is also an option, which targets visible blood vessels, improves skin texture, and tone.
Although living with rosacea can be challenging, with proper care and treatment, patients can keep the symptoms under control. If you are struggling with rosacea, at schedule an appointment with Dr. Neily at Coast Dermatology in Venice, FL. He can help you develop a customized treatment plan that works for you, allowing you to manage your rosacea and take back control of your life.















